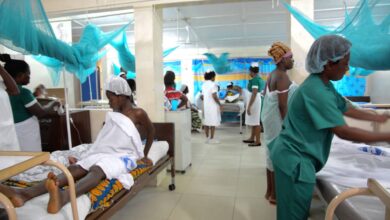
New CHPS Facility, WASH Investment Highlight Growing Role of Partnerships in Closing Rural Healthcare Gaps
Limited access to basic healthcare and sanitation continues to define life in many rural communities, forcing greater reliance on partnerships between government and non-state actors to close critical service gaps.
That reality was on display in the Mfantseman Constituency, where The Church of Jesus Christ of Latter-day Saints has financed and delivered a new Community Health Planning and Services (CHPS) compound at Daadagua, alongside water, sanitation and hygiene infrastructure aimed at improving public health outcomes.
The intervention reflects a broader trend: essential services in underserved areas are increasingly being sustained through external support rather than public investment alone.
Filling a Critical Gap
The CHPS compound is expected to serve as a frontline facility, providing preventive, promotive and basic curative care to residents in Daadagua and surrounding communities.
Under Ghana’s community-based health model, such facilities are designed to reduce pressure on district hospitals while improving early access to care. But in many parts of the country, infrastructure deficits have limited the effectiveness of the system.
Municipal Health Director Gifty Ankrah said the new facility addresses a longstanding coverage gap, noting that operational capacity in the CHPS system is often constrained by the absence of functional infrastructure.
The Ghana Health Service is expected to take over staffing and management of the facility, underscoring the hybrid model where private capital delivers infrastructure and the state provides service continuity.
Sanitation and Water: The Missing Link
Alongside the clinic, the project includes a borehole and a ten-seater sanitation facility—interventions that directly target water and hygiene challenges that continue to undermine health outcomes in rural communities.
In areas where access to clean water remains inconsistent, preventable diseases linked to poor sanitation still impose economic and social costs, particularly on households and local health systems.
The integration of WASH infrastructure into the health project reflects growing recognition that healthcare delivery cannot be separated from environmental conditions.
Partnership as Development Model
The project was delivered in collaboration with local authorities, including Member of Parliament Ebenezer Prince Arhin, highlighting the increasing role of constituency-level partnerships in driving development.
For policymakers, this model presents both an opportunity and a challenge.
On one hand, partnerships with faith-based organisations and development actors can accelerate infrastructure delivery. On the other, it raises questions about the sustainability and scalability of relying on external actors to fund core public services.
Traditional authorities also signalled the importance of local ownership. Anomabo Omanhene Nana Kantamanto Amonu stressed the need for communities to maintain and protect the facilities, pointing to a recurring issue where infrastructure deteriorates due to weak local stewardship.
A Broader Strategy
Representing the Church, Isaac K. Morrison said the initiative forms part of a wider humanitarian strategy focused on sustainable, community-driven development.
The Church’s approach, funding infrastructure while working through public institutions aligns with a growing emphasis on long-term impact rather than one-off interventions.
The Bigger Picture
Ghana’s CHPS model remains central to expanding primary healthcare, but its success continues to depend on infrastructure, staffing and sustained financing.
Projects like Daadagua’s clinic illustrate how targeted investments can unlock the system’s potential. But they also highlight the underlying issue: without consistent public funding, progress will remain uneven.
Bottom Line
The new CHPS facility and WASH infrastructure in Mfantseman are more than community projects—they are a reminder that closing Ghana’s healthcare gaps increasingly depends on partnerships.
The long-term test will be whether such interventions can be scaled, sustained and integrated into a broader strategy for equitable service delivery.